Whether you are experiencing symptoms of peripheral artery disease (PAD) or have been told you are at an increased risk, it’s important to know how your genes impact the likelihood of certain conditions.
In the past, your doctor may have told you that brushing up on your family’s health history is an important thing to do, especially as you get older. One of the most beneficial and proactive things you can do for your health is to rule out hereditary risk factors that could increase the likelihood of developing PAD.
What Risk Factors Make Peripheral Artery Disease Hereditary?
As you may already know, various hereditary risk factors that may run in your family can increase your risk of developing PAD. These may include:
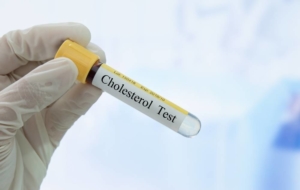
- High blood pressure or cholesterol levels
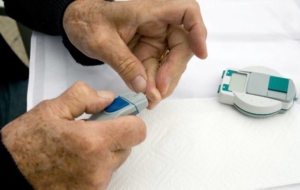
- Diabetes
- Family history of vascular disease
- Secondhand smoke inhalation
- History of a stroke or heart attack
These risk factors increase your risk by inhibiting plaque buildup within the arteries, especially those located in your legs.
If you’re concerned about one or more of the above risk factors, give our vascular specialists a call at 888.773.2193 or contact us online to schedule an initial consultation. As we delve into each risk factor, you will see how each can contribute to the development of PAD.
High Blood Pressure and Heredity
High blood pressure, also referred to as hypertension, is one of the most common risk factors of peripheral artery disease. This is because it makes it easier for your body to accumulate plaque within your arteries. Sustained blood pressure levels over time can lead to strokes, heart attacks, and yes, PAD.
You may be wondering, “why is high blood pressure hereditary”? Unfortunately, it isn’t the easiest of questions to answer. High blood pressure tends to run in families and is caused by gene mutations. This may be because families often share common environments and other potential factors that increase their risk. However, you can still break the cycle. Even though you may feel like you can’t control your genes, high blood pressure is a risk factor that can be effectively managed with exercise, diet, and medication.
Diabetes and Your Genes
Another risk factor of PAD is having type 2 diabetes. If type 2 diabetes is not effectively managed, high blood sugar levels can cause the arterial walls to become rough. This allows plaque to easily attach itself and accumulate along the sides of the arterial walls.
Although type 2 diabetes isn’t always inherited, many people who have this condition often have a parent or sibling that also does. If you’re wondering, “is type 2 diabetes hereditary?” the answer is, yes, it can be. Talking to your doctor about how to manage inherited type 2 diabetes is crucial for preventing PAD.
Genetic Vascular Disease
This one is pretty straightforward. If you have a family history of any kind of vascular disease (coronary, carotid, claudication, DVT, superficial blood clots, aneurysm, etc.) you may have an elevated risk of developing PAD. Many genetic vascular diseases are caused by blood not having the ability to transport freely throughout the body. These issues are often caused by either a heart or arterial issue. When blood is not circulating through your body to your lower extremities, PAD can develop.
Even though it may seem predisposition is inevitable, genetic vascular disease can be avoided by taking a few precautions. Consulting your doctor regularly, getting an ankle-brachial index (ABI) test, and exercising can help lower your risk of genetic vascular disease turning into PAD. If you are aware of genetic vascular diseases running in your family, consult a specialist immediately.
Elevated Cholesterol and Potential Risks
High cholesterol over a long period of time without management is the number one reason for plaque buildup within the arteries. If you know you have a history of high cholesterol in the family, you need to be proactive about what foods you consume. So, how do you beat hereditary high cholesterol? Well, avoiding foods such as sausages, fried food, red meat, and sweets will help lower cholesterol levels that may put pressure on your arterial walls.
But, is high cholesterol hereditary? Yes. Even if you avoid these cholesterol-rich foods, you may not be out of danger. Your body may be more accustomed to overproducing cholesterol if a family member like a parent or grandparent has had an issue with it in the past. This can also lead to a plaque buildup with your arteries, causing narrow passageways. When your blood is unable to successfully transport blood, oxygen, and nutrients to your extremities, issues like heart attacks, strokes, and gangrene could arise.
Heart Attack and Stroke Risk Factors: Genetics and Prevention
Unlike other PAD risk factors that directly correlate with one another, having a family history of heart attacks or strokes may not seem connected, but they are. So, even if you take all the necessary precautions, are strokes genetic? They can be. If you are predisposed to have narrowing of the arteries, pr poor circulation, strokes and heart attacks could be genetic.
Are heart attacks hereditary as well? Yes, because oftentimes they are caused by the same inherited issues. On the other hand, if you have already had a heart attack or stroke, your heart has most likely suffered damages and stress from going through that ordeal. Even if you had a heart attack or stroke years ago and have fully recovered, your heart’s rhythm and ability to pump blood could be insufficient. If your heart cannot successfully pump blood to your lower extremities, you may develop PAD symptoms.
Heart attack and stroke risk factors shouldn’t be taken lightly or ignored. These can lead to serious, life-threatening conditions like PAD.
How to Be Proactive About Peripheral Artery Disease
Being proactive about your health starts at understanding your family’s health history. If you find out someone in your family such as a mother, father, or grandparent has had vascular disease, high cholesterol, hypertension, diabetes, stroke, heart attack, or PAD, consult your physician to learn how you can reduce your risk.
The first part is to listen to your body and start good habits. Exercising regularly, eating a balanced diet, as well as managing stress, can help prevent plaque buildup from increasing. The second is treating PAD as early as symptoms arise. Inform your doctor and find a vascular specialist if you are experiencing any of the following:
- Fatigue, heaviness, tiredness in one or both of your legs
- Leg cramping in the leg muscles, buttocks, thigh, or calf
- Difficulty climbing stairs
- Restless or painful legs during sleep
- Slow or non-healing wounds on the legs or feet
- Color changes in the skin of the feet, including paleness or blueness
- A lower temperature in one leg compared to the other leg
- Poor toe nail and leg hair growth
- Leg pain that stops when at rest
PAD can be life-threatening if ignored, leading to stroke, heart attack, or amputation. Thankfully, there is an outpatient, nonsurgical treatment that can be used to unblock clogged leg arteries called stent angioplasty.
Whether you have already been diagnosed or are just starting to experience symptoms USA Vascular Centers can help. Give us a call at 888.773.2193 or schedule with one of our vascular specialists online for an initial consultation.