Did you know that poor circulation when sleeping can be linked to peripheral artery disease (PAD)?
When PAD causes the arteries to narrow, it reduces blood flow to the legs and leads to symptoms such as leg pain or cramping while walking. In earlier stages, the pain typically improves with rest. As the condition progresses, the pain may persist despite resting and may become more noticeable at night.
PAD can worsen over time due to various factors, such as smoking, high blood pressure, high cholesterol, and diabetes. Multiple studies also suggest that sleep apnea may contribute to PAD’s progression.
Sleep apnea disrupts breathing during sleep, lowering oxygen levels and placing repeated strain on the heart and blood vessels. Over time, this can contribute to changes in the arteries and poor circulation when sleeping, increasing the likelihood of .
Understanding the connection between sleep apnea and PAD can help explain why symptoms may appear or worsen at night—and when it’s time to seek a medical evaluation.
Understanding the Link Between Sleep Apnea and PAD
Sleep apnea and PAD are two conditions that affect the body differently but can be connected through their impact on circulation.
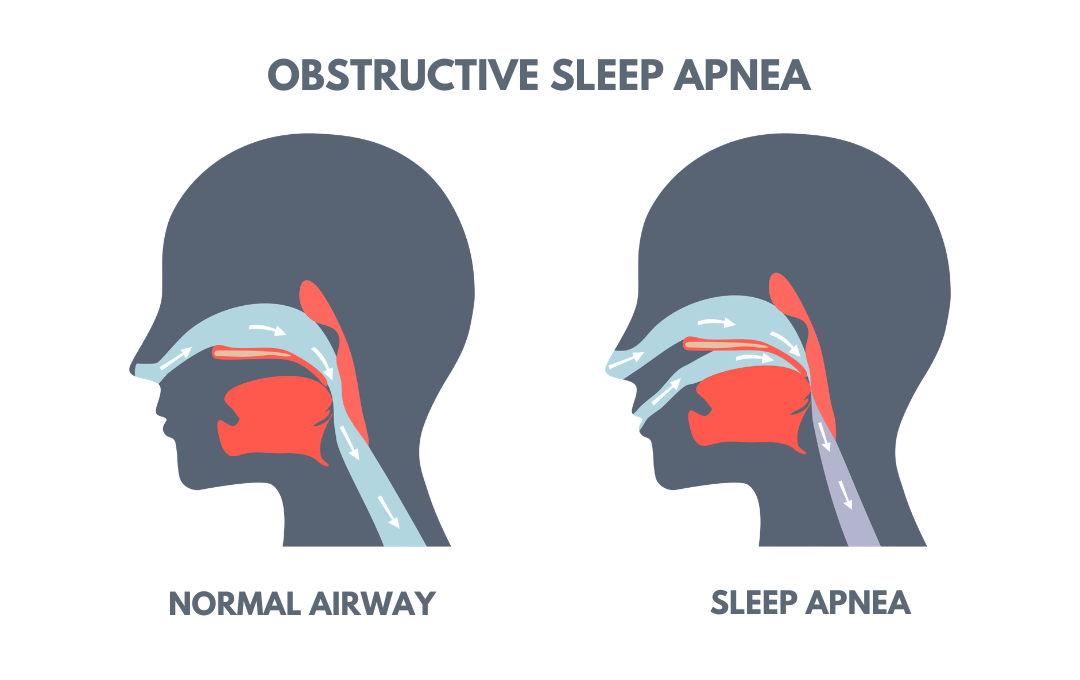
Sleep apnea is a sleep disorder where breathing repeatedly stops and starts due to airway obstruction or disrupted brain signals. These interruptions can occur dozens or even hundreds of times in a single night. Common signs include loud snoring, waking up gasping for air, morning headaches, and daytime fatigue. The risk of sleep apnea increases for people who are over the age of 65, overweight, or male.
Peripheral artery disease (PAD) is a narrowing of the arteries due to a buildup of plaque, a combination of cholesterol and other fatty substances that stick to the arterial walls. As plaque builds up gradually, the arteries will narrow and reduce blood flow to the limbs, most commonly the legs. This can cause symptoms such as leg pain during walking, cramping, or slower healing in the lower extremities.
How Poor Circulation in the Legs Disrupts Your Sleep
Common signs of poor blood circulation in legs while sleeping include:
- Leg discomfort or aching at night
- Tingling or numbness in the feet or legs
- A feeling of heaviness in the lower legs
- Cold feet despite a warm environment
- Cramping that occurs during rest
In patients with sleep apnea and PAD, symptoms may be more difficult to manage. Sleep apnea can lead to poor sleep quality and daytime fatigue, which may reduce physical activity. Since regular movement helps support blood flow in the legs, lower activity levels may worsen symptoms over time.
Explore the Best Sleeping Positions for PAD
Can Sleep Apnea Cause PAD?
While sleep apnea does not directly cause PAD, it can contribute to the development of the disease. Research from the National Institutes of Health and the American Heart Association has found that sleep apnea could increase the risk of PAD between 37 and 60 percent. Additional research has also found a higher prevalence of sleep apnea in patients with advanced PAD.
How Sleep Apnea Can Affect Circulation and Blood Vessels
When sleep apnea interrupts breathing, it lowers oxygen levels in the body. As a result, heart rate increases, and blood vessels tighten. This response is meant to protect vital organs, but when it happens repeatedly, it can affect how blood flows through the arteries.
Sleep apnea and poor blood flow can contribute to inflammation over time, elevating blood pressure and damaging the arteries. Damaged arteries can make plaque buildup more likely and increase the risk of conditions like PAD.
Are You At Risk? Take Our Quiz
When to Seek Medical Attention
Physicians at USA Vascular Centers advise that any symptoms of PAD, such as leg pain, numbness, or cold feet, should be screened. When these symptoms start to impact sleep, it may indicate that PAD has advanced to more serious stages, emphasizing the need for treatment to reduce the risk of complications.
If left untreated, PAD may lead to more persistent pain, limited mobility, and slower healing in the legs. An early screening can help identify poor circulation early and allow timely treatment to prevent symptoms from progressing.
How Sleep Apnea and PAD Are Diagnosed
Sleep apnea and peripheral artery disease are diagnosed through different methods. Sleep apnea is typically diagnosed through a sleep study, which monitors breathing, oxygen levels, and sleep patterns overnight.
PAD is often detected through non-invasive tests that measure blood flow in the legs. These tests include:
- Ankle-Brachial Index (ABI): Compares the blood pressure in your arms and your ankles.
- Ultrasound: Uses sound waves to visualize blood flow in the arteries.
- Angiography: Involves injecting a specialized contrast dye and using X-ray imaging to locate blockages in the arteries.
Once PAD is diagnosed, the screening results will guide vascular specialists in selecting the most appropriate next steps for patients.
Next Steps for Managing Sleep Apnea and PAD
Patients with sleep apnea are advised to see their primary care physician or a sleep specialist for tips on managing the condition. This may include treatments, such as continuous positive airway pressure (CPAP) therapy, to support breathing overnight.
PAD treatments are focused on restoring blood flow to the limbs and managing symptoms to slow the disease’s progression. These treatments are tailored based on the severity of PAD, which may include:
- Lifestyle changes, such as supervised exercise therapy
- Medications to manage high blood pressure and cholesterol
If symptoms continue or worsen, minimally invasive procedures may be recommended to open the arteries and improve blood flow. USA Vascular Centers offers these treatments on an outpatient basis, allowing patients to return home the same day with minimal disruptions to their daily routine.
Don’t Ignore Ongoing Poor Circulation When Sleeping
If you’re experiencing ongoing leg pain, cramping, or discomfort that affects your sleep, it’s important not to ignore these symptoms.
While managing sleep apnea, poor blood flow, and other risk factors can support overall health, targeted treatment for PAD may be needed to improve blood flow and relieve symptoms.
At USA Vascular Centers, we offer comprehensive vascular care for patients struggling with PAD. Our vascular specialists use advanced imaging techniques to evaluate blood flow and accurately identify arteries narrowed by the condition. Because PAD can lead to serious complications, PAD treatments are generally covered by many health insurance plans. Patients can verify their coverage when they schedule their appointment online or by calling (888) 773-2193.
If you’re concerned that PAD is interrupting your sleep, schedule a consultation with USA Vascular Centers today.
Frequently Asked Questions (FAQs)
Can sleep apnea cause peripheral artery disease?
Sleep apnea does not directly cause PAD, but it is associated with a higher risk of developing the condition. Research shows that sleep apnea can contribute to changes in the cardiovascular system that may increase the likelihood of narrowed arteries over time.
What does sleep apnea do to the blood?
Sleep apnea causes repeated interruptions in breathing during sleep, which can lower blood oxygen levels and put additional strain on the heart and blood vessels over time.
Can sleep apnea cause poor blood circulation?
The repeated oxygen dips caused by sleep apnea can contribute to poor circulation when sleeping and act like a physical toll on the vascular system. Over time, this constant fluctuation damages the lining of the arteries, making it harder for blood to circulate efficiently to the extremities.