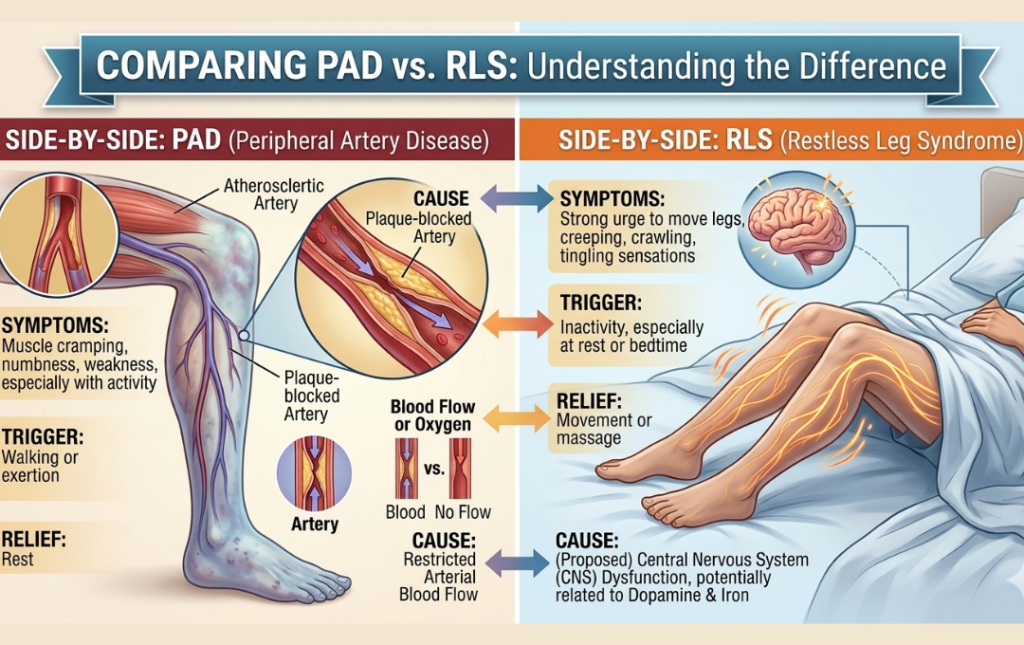
Tossing and turning with a “creepy-crawly” feeling in your calves, or having to stop in the middle of your walk due to sudden cramping, can be more than frustrating. When it comes to peripheral artery disease (PAD) vs. restless leg syndrome (RLS), while both cause aching and unusual sensations, they stem from very different sources.
Understanding the difference between RLS and PAD is important, as one affects your sleep while the other may require a vascular evaluation for your circulatory health. Here is how to recognize the overlapping symptoms and identify when your discomfort is a sign of poor circulation.
Why PAD and Restless Leg Syndrome Can Feel Similar
When you are dealing with persistent leg discomfort, pinpointing the cause can be hard because the sensations often overlap. This is especially true when comparing Restless Leg Syndrome (RLS) and Peripheral Artery Disease (PAD).
- Restless Leg Syndrome (RLS) is a neurological condition that causes an irresistible urge to move your legs, typically while you are resting or trying to sleep.
- Peripheral Artery Disease (PAD) is a vascular condition where narrowed arteries restrict blood flow to your lower limbs, usually causing pain or cramping during physical activity.
Both conditions can manifest as a deep aching, throbbing, a “pins and needles” sensation, or a general sense of unease in the lower limbs, making them incredibly easy to confuse.
Furthermore, both PAD and RLS can severely disrupt your sleep, causing intense leg discomfort at night. However, poor circulation (PAD) is more likely to be the underlying driver of your symptoms if your nighttime discomfort is accompanied by:
- A persistent feeling of heaviness in the calves or thighs
- Frequent, painful charley horses or cramping
- Feet or toes that feel unusually cold to the touch compared to the rest of your body
The Hidden Trigger: Anemia
To complicate matters further, anemia, a condition where your body lacks enough healthy red blood cells to carry oxygen to your tissues—plays a major role in how these symptoms mimic one another. Iron deficiency anemia is a well-known medical trigger for Restless Leg Syndrome. When you are anemic, your leg muscles do not receive the optimal amount of oxygen they need to function properly at rest, prompting those frustrating, crawling RLS sensations.
While PAD starves your legs of oxygen due to restricted blood flow, anemia starves them of oxygen due to poor blood quality. Because the root result for your muscles is exactly the same—a critical lack of oxygen—an anemic patient experiencing RLS can easily mistake their symptoms for a circulation issue like PAD.
Timing and Triggers: How to Tell Them Apart
While the physical sensations are quite similar, the timing and triggers of the pain are your most important clues.
Understanding exactly when your symptoms happen—whether they strike only when you are completely still or flare up the moment you start moving—is the first step in separating a neurological issue from a vascular blockage. By looking closer at the specific triggers of restless leg syndrome vs. peripheral artery disease, you can better identify whether your legs are simply restless or if they are signaling a deeper issue like atherosclerosis.
PAD vs RLS Symptoms: How to Tell the Difference
The primary difference between RLS and PAD is how your body reacts to movement. If you feel an overwhelming, jittery urge to kick or shift your legs while sitting or lying down and that feeling improves the moment you get up and pace, you are likely experiencing restless leg syndrome.
On the other hand, PAD pain, known as claudication, usually strikes when you are active. You might feel a heavy, tight cramping in your calves or thighs while walking that only subsides once you stand still and rest. While advanced PAD can cause pain at night, it is often relieved by hanging your legs over the side of the bed to let gravity assist your circulation, whereas RLS symptoms generally worsen with any form of rest. Recognizing these patterns is the most effective way to determine if your discomfort is neurological or vascular.
Symptoms of Peripheral Artery Disease in Legs
Recognizing the specific symptoms of peripheral artery disease in the legs is essential because, unlike neurological issues, PAD is rooted in physical blockages. The biggest sign of PAD symptoms is claudication—muscle pain or cramping that occurs during activity and disappears with a few minutes of rest. Since the narrowed arteries cannot deliver enough oxygen-rich blood to the muscles during exertion, the legs begin to protest.
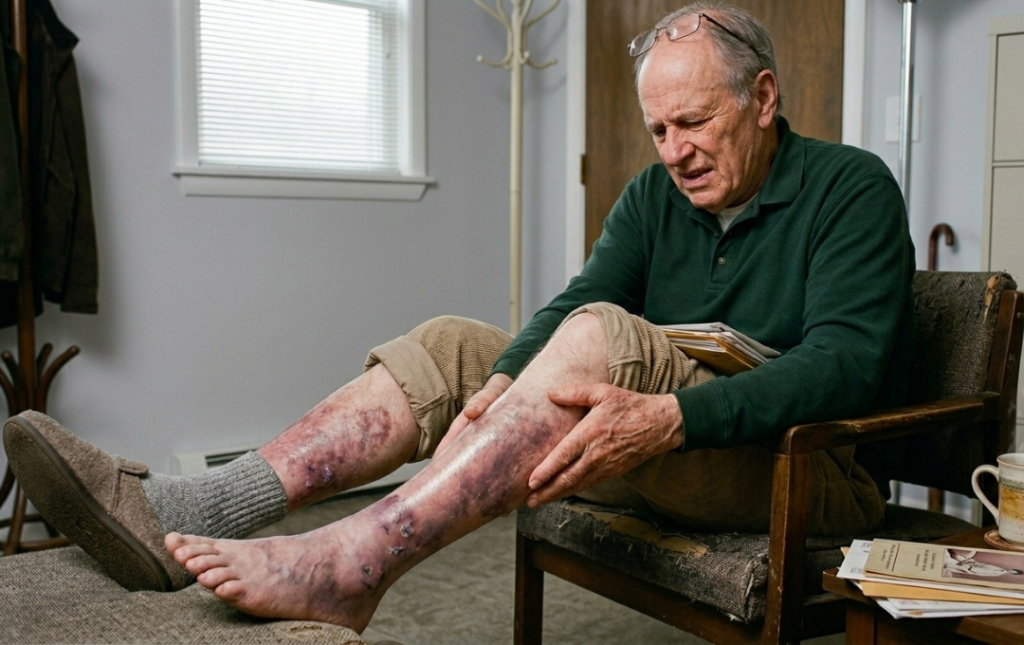
So, what does PAD leg pain feel like? Many describe it as a heavy, tight, or “knotting” sensation, most commonly felt in the calves, thighs, or buttocks while walking or climbing stairs. Beyond the pain, you might notice physical changes such as skin that feels cool to the touch, a shiny appearance on the shins, or hair loss on the feet and ankles. In more advanced stages, the lack of circulation can lead to sores on the toes or feet that are slow to heal, signaling that the vascular system requires immediate attention.
Key Symptoms of Restless Leg Syndrome
Identifying the symptoms of restless leg syndrome often starts with a very specific, almost indescribable feeling. Most people describe it as a “creepy-crawly” feeling, itching, or pulling deep within the muscles. Unlike a standard muscle cramp, restless leg syndrome feels like an overwhelming, involuntary urge to move the limbs to find temporary relief.
While the sensations themselves are uncomfortable, the timing is the most distinct of all restless leg syndrome symptoms. These urges typically intensify in the evening or late at night, specifically during periods of inactivity. Whether you are sitting through a long movie or tucked into bed, the discomfort tends to vanish the moment you get up and walk around, only to return once you settle back down. This cyclical nature is a hallmark of the condition, distinguishing it from other types of chronic leg pain.
When Poor Circulation Could Be the Common Denominator
Many people find themselves questioning the link between restless legs vs. poor circulation. It is common for vascular health to be overlooked when the symptoms involve fidgeting or mild aching, but restless legs syndrome and poor circulation are often more connected than they appear. In some cases, what feels like a nervous urge to move may actually be a response to the heavy, sluggish feeling caused by restricted blood flow.
Distinguishing poor circulation vs. restless legs is essential because vascular issues like PAD can mimic the discomfort of RLS while requiring a completely different medical approach. If your leg sensations are accompanied by physical signs like skin discoloration, sores that won’t heal, or a noticeable drop in skin temperature, it is a strong indicator that the issue is circulatory. Recognizing these signs helps determine if your discomfort is a byproduct of a restless nervous system or a sign that your arteries need specialized attention.
What Causes Restless Legs vs. PAD?
While Restless Leg Syndrome (RLS) is caused by a chemical glitch in your nervous system, Peripheral Artery Disease (PAD) is caused by a physical blockage in your blood vessels. To find the right treatment, it is essential to look at how differently these two underlying systems operate.
Restless leg syndrome causes are primarily neurological. Researchers believe the condition is linked to an imbalance of dopamine, a brain chemical that manages muscle movement. This imbalance is often what causes restless legs at night; as your body settles into a resting state, the brain sends erratic signals to the limbs, creating that urge to move.
In contrast, PAD causes are physical and circulatory. Peripheral artery disease stems from , where fatty plaque builds up on the artery walls and narrows the path for blood flow. While this usually causes pain during activity, it can also lead to PAD symptoms at night. When you are lying flat, your heart has a harder time pushing oxygen-rich blood through narrowed vessels to your feet without the help of gravity.
When Leg Symptoms May Be a Warning Sign of PAD
Even though occasional leg fatigue is common, certain signs of peripheral artery disease serve as red flags for poor circulation. Unlike the twitching of RLS, PAD warning signs often follow a progressive pattern that indicates how severely your blood flow is restricted.
In the early stages of PAD, you might notice “claudication”—a specific type of muscle pain or cramping that appears during movement, such as walking or climbing stairs, but disappears quickly with rest. However, as the disease advances, your legs may begin to show visible changes. Keep a close watch for these symptoms:
- Skin and Nail Changes: Legs may appear shiny, or the skin may take on a bluish or pale hue. You might also notice slower hair growth on your legs or brittle toenails.
- Temperature Differences: One foot or leg may feel significantly colder to the touch than the rest of your body.
- Non-Healing Sores: Small cuts, scrapes, or ulcers on your feet or toes that refuse to heal are serious indicators of poor nutrient delivery to the tissues.
- Persistent “Rest Pain”: Feeling a dull ache or burning sensation in your toes while lying in bed is a sign that the blockage is significant enough that even gravity’s help is needed to move blood to your extremities.
Ignoring these signals can lead to more severe complications, such as critical limb ischemia. If any of these physical changes accompany your leg discomfort, it is a clear indication that the issue is PAD rather than RLS, making a medical evaluation necessary.
How PAD and Restless Leg Symptoms Are Diagnosed
A professional evaluation is the only way to accurately confirm a restless leg syndrome vs. peripheral artery disease diagnosis. Since the two conditions require different medical specialties—neurology and vascular medicine—doctors use distinct diagnostic tests to identify the source of your discomfort.
When determining if you have PAD or restless leg syndrome, the RLS process is primarily clinical. A doctor will review your history to see if your symptoms worsen during rest, occur mainly at night, and are relieved by movement. Since there is no specific blood test for RLS, your description of the “urge to move” is the primary diagnostic tool.
For diagnosing PAD, a PAD vs. restless leg diagnosis relies on objective physical tests. A vascular specialist will typically perform an ankle-brachial index (ABI), which compares the blood pressure in your ankles to the pressure in your arms. If blood flow appears restricted, they may use a Doppler ultrasound to visualize plaque buildup within the arteries. These tests allow doctors to see physical blockages that a standard neurological exam might miss, ensuring you receive the correct treatment for your circulatory health.
Treating Leg Symptoms Starts With the Right Diagnosis
Effective relief depends entirely on addressing the source of the discomfort. Restless leg syndrome treatment focuses on calming the nervous system and improving sleep. This often includes lifestyle changes like reducing caffeine, establishing a consistent sleep schedule, and moderate exercise. In some cases, doctors prescribe medications to regulate dopamine levels or address iron deficiencies to reduce the urge to move.
PAD treatment, however, is focused on restoring blood flow. While lifestyle adjustments like specialized walking programs and cholesterol management are vital, advanced cases may require minimally invasive procedures. Techniques such as angioplasty, stenting, or atherectomy physically clear plaque from the arteries to improve circulation. Starting with the correct diagnosis ensures you are pursuing a path that actually resolves the underlying issue rather than just managing the sensations.
Get Answers at USA Vascular Centers
If you are unsure whether your leg discomfort is restless leg syndrome or peripheral artery disease, USA Vascular Centers can provide the clarity you need. Our specialists are experts in distinguishing RLS vs. PAD, using advanced diagnostic tests to identify if poor circulation is the actual cause of your symptoms.
Our AAAHC-accredited centers are led by board-certified physicians who prioritize patient safety and effective results. We offer personalized treatment plans designed to restore blood flow and improve your quality of life. We accept most insurance plans and can verify your coverage during the scheduling process. Schedule a consultation today to determine if your symptoms require treatment for PAD.
Meet A Vascular Specialist Today
FAQs
Does PAD feel like restless leg syndrome?
PAD can feel like restless leg syndrome because it can cause similar aching and pins and needles.
What stops restless leg syndrome immediately?
To stop restless leg syndrome immediately and achieve long-term relief requires addressing underlying causes, such as iron deficiencies or neurological imbalances. Walking, stretching, or shaking the legs can provide fast, temporary relief for restless leg syndrome.
What is mistaken for restless leg syndrome?
Peripheral artery disease (PAD), peripheral neuropathy (nerve damage), venous insufficiency, or simple muscle cramps are often mistaken for restless leg syndrome. Because symptoms overlap, objective testing is required for an accurate diagnosis.
Does peripheral artery disease cause restless legs?
Peripheral artery disease (PAD) does not cause restless legs. However, PAD causes “rest pain” at night due to poor circulation, which creates a feeling of leg agitation that mimics the sensations of restless leg syndrome.